First Steps Guide
First Steps Guide
First Steps Guide
First Steps Guide
Click a step below to learn more
Welcome to our First Steps Toolkit
Welcome to our First Steps toolkit - a resource designed to help parents and carers of autistic children to navigate their journey in the early years. These days there is a staggering amount of information about autism available online, in books or through word of mouth. Much is reliable, some less so - but the sheer volume of information can feel overwhelming, difficult to sift through and hard to verify. This is why Autism Edmonton has created this toolkit - to provide practical and straightforward information in one place that will guide families with young children through their autism journey.
Although every effort has been made to describe this journey accurately, we know that, at times, your own 'journey' may be very different. This toolkit should therefore be considered a 'guide book' rather than a timetable - one that has been designed to be helpful and relevant for your travels, whatever stage you are at. We use the word 'parent' throughout the toolkit but we understand that the range of people caring for a young child is much broader than that. By 'parent' we mean any primary carer of a young child, including adoptive or foster parents.
The sooner you understand your child's needs, the sooner they will have the support they need. Early identification of your child's needs and early intervention (therapies and support strategies) can provide:
- a better understanding of your child and how best to help them
- access to the correct services and supportive educational settings
- knowledge of the skills needed to enhance your child's education, friendships and quality of life
- a chance to prepare yourself emotionally and mentally for the future
- the opportunity to take advantage of early brain development, maximising the potential impact of interventions
- an opportunity to get the support your child needs to help them learn and develop to be ready for school and adult life.
Autism is not a disease. It is a neurological condition.
It is also a developmental disorder - something a person is born with and which impacts them across their whole life. Together, these categories mean that autism is often referred to as a neurodevelopmental condition. It is something you can't change and there is no cure for autism.
Autism is also a spectrum condition, meaning that people with autism share certain characteristics but are also highly individual in their needs and preferences.
As a parent, it's important to understand not only what autism is defined as, but what being autistic means for your child.
Qualified healthcare professionals use diagnostic tools to make medical assessments as well as the DSM-V, the fifth edition of the Diagnostic and Statistical Manual, which outlines the criteria diagnostic professionals use to decide if autism is the right description of the difficulties the person is experiencing.
According to the CDC, 1 in 44 are autistic. It is not a disease, but a neurological condition that impacts the way a person communicates and how they experience the world around them.
The DSM-V describes autism as a disorder that impacts a person's communication skills and social interactions, including repetitive behaviours and activities. In addition, the DSM-V says that there should be evidence of 'persistent' difficulties across more than one of the following categories:
- Communication differences: difficulties using and interpreting speech, written words, and non-verbal language such as gestures.
- Social interaction differences: difficulties expressing emotion and recognising or understanding the feelings and intentions of others ('reading' other people).
- Repetitive behaviors and activities: being highly focused on particular subjects, objects, routines, and rituals.
It is also common for autistic individuals to have difficulty dealing with and processing sensory information - the information their senses send to their brain. If a sense is 'turned up' (hypersensitivity), they might become overstimulated by situations and environments that can cause sensory overload. In situations like this, if the child is made to remain in the overwhelming environment, it could potentially lead to something known as a 'meltdown'.
A meltdown is defined as 'an intense response to overwhelming situations'. A meltdown happens when someone becomes completely overwhelmed by their current situation and temporarily loses behavioural control. This loss of control can be expressed verbally through shouting, screaming or crying; physically by kicking, lashing out or biting; or in both ways.
If their senses are 'turned down' (hyposensitivity), they may not react to their sensory environment or seem unaffected by sometimes quite dangerous environments. Some autistic children can also be 'sensory seeking', which means they seek out sensory stimulation because they like the sensation of particular sensory inputs.
Repetitive behaviours are also a common feature of autism in children and young people. They can be an essential way of regulating emotion, providing someone with a source of comfort or enjoyment, and enabling them to carry on with their day
The common name for repetitive behaviours in autistic people is 'stimming' - short for 'self-stimulatory behaviour'. Some forms of stimming are barely noticeable, and some are very visible. They vary in frequency and appearance, depending on the person. Stimming can help autistic people regulate their emotions and process their sensory environment.
Stimming is often an autistic person's way of managing a situation and reducing stress; as such, it shouldn't be stopped or reduced. However, stimming can sometimes cause self-injury, for example through headbanging or scratching.
Some forms of repetitive behaviours are often linked to the senses, for example:
- Visual: staring at spinning objects; staring at lights; doing things to make the vision flicker such as repetitive blinking or shaking fingers in front of eyes.
- Tactile: rubbing the skin with hands or with another object; scratching.
- Auditory: listening to the same song or noise on repeat or making vocal sounds; tapping ears and snapping fingers.
- Taste/smell sniffing objects or people; licking or chewing on things that often aren't edible.
- Proprioception this is the body's ability to feel where it is and what it's doing. This could present in behaviour such as rocking, swinging, jumping, pacing, running, tiptoeing or spinning - all of which give the body's sense of balance and position a boost. Some autistic children enjoy the sensation of pressure.
Autism is many things but, put simply, it is a different way of viewing and experiencing the world. It is important to understand how autism applies to your child, including their skills and talents. It's also important to encourage and nurture your child in the things they are good at, as well as supporting them with any difficulties they face. As a parent you may automatically do this, but it may be good to emphasise your praise and support.
Autism as a 'spectrum'
Because there are different levels of complexity, autism is often described as a spectrum. The term 'autistic spectrum disorder' (ASD) is, in fact, often used. But this suggests that autism is a simple sliding scale like this:
This is misleading. Autism is not a linear scale like this, and we shouldn't place autistic people on a scale based on our assumptions about their abilities. It is more accurate to say that autism might influence some areas of the brain while other areas will be no different from an average, or 'neurotypical', person.
To visualise this more clearly, the spectrum can be thought of as a colour wheel, where characteristics like motor skills and language blend together like the colours of a rainbow:
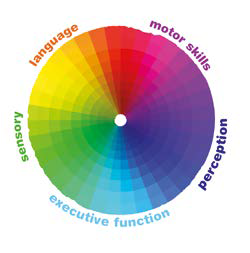
Everyone is different. Some people have highly developed skills in certain areas, while other people find those same things challenging. In the case of motor skills for instance, there are people who can assemble the fine parts of a watch while others may struggle to thread a needle. But let's assume on our wheel, the watchmaker is shown with the green dot and the person who struggles to thread a needle would be the black dot.
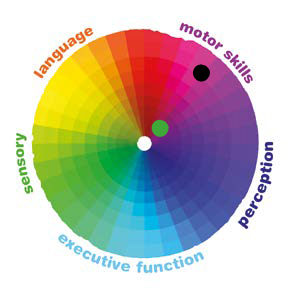
Everyone will have different abilities and skills in different areas of the wheel. For example, one person may be very good at making conversation (language) but may experience sensory overload in loud and crowded spaces. It may be that they function no differently in all other areas. If this was mapped out, it would look like the spots in this wheel:
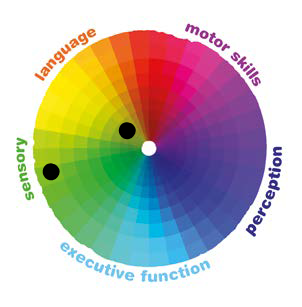
Another person might be happy in loud crowds but find conversation hard, which would look like this:
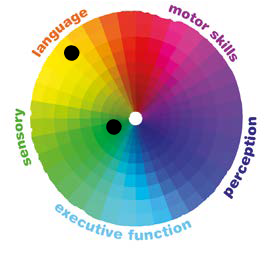
Seeing the spectrum in this way illustrates that difficulties in one area don't define a person's skills in all areas. For example, someone who is not good at communicating verbally may just need a different way to communicate. This approach also shows how some autistic individuals might have highly developed skills in certain areas, such as memory, observing fine detail or knowledge of a particular subject, even though their autism may lead to difficulties in other areas.
So, seeing the spectrum in this way shows that an autistic person is not simply a 'little bit' or 'very' autistic. Autistic individuals can have significant strengths while feeling challenged in other areas. Remember that the DSM-V says that a criteria for diagnosing autism is 'persistent difficulties' across more than one area.
Autism and girls
Research suggests that four times as many boys are diagnosed with autism as girls. But many think the actual number of autistic girls is likely to be much higher.
The ways in which autism manifests in girls remains under-researched, but we know that girls often display autistic traits in subtler ways than boys.
For example, girls are more likely to take part in imaginative or pretend play, such as playing tea parties with dolls, which is a type of play autistic children may often find difficult. However, in autistic girls, this type of play is often learnt by watching other children and they tend not to go on to develop their own play sequences.
Autistic girls also often have better language skills than autistic boys and their restricted interests may be less obvious (for example, animals or people such as TV characters, rather than objects).
Girls are less likely than boys to show sensory-seeking, repetitive behaviours. There is also research that suggests, perhaps because of greater societal expectations, that many girls try to mask their difficulties, for example by copying the behaviour and appearance of other girls.
Autistic girls can often need a lot of downtime to recover after socialising, as masking and compensating can be very tiring.
All of these aspects can make it harder to identify autistic traits in girls, especially if they don't have additional challenges such as a language delay. It is often said that assessment and diagnostic tools are biased towards boys, in part because most research into autism and how to diagnose it has focused on boys. When a GP, teacher or health worker sees a girl who is socially different, they may be less inclined to wonder whether it could be autism than in the case of a boy. Other difficulties, such as eating disorders or anxiety, may be diagnosed, while autism is overlooked. This has meant that, in many cases, girls do not receive assessments, diagnosis or support until they are much older.
There is increasing awareness about autism in girls and women but, if you have a daughter with suspected or confirmed autism, you may have to work a little harder at making sure your daughter's difficulties are recognised and supported by you, your family, friends and others in her childcare or educational environment.
Could my Child be Autistic?
Understanding your child

Your child's speech, language and social skills are a useful indicator of their developmental progress. Speech and communication development is not just about using more and more words. It is also about understanding how words are used, for example that '...where is mom?...' is a question requiring a response. It is also about how children interact with the people around them; such as asking for things, telling you what they want, and forming relationships with other children and adults.
By the time they are two years old most children will have begun to understand and use simple words that they hear often, such as 'Mommy', 'Daddy', 'ball' and 'teddy'. They will start to take an interest in naming or understanding parts of the body, such as the eyes, head, and toes. They will begin to understand that words are linked to activities - for instance, that 'yummy' and 'lunch' are linked to eating, or that 'bedtime' and 'tired' are linked to sleeping. They will have probably started to use gestures such as pointing or shaking their head to mean 'no'.
Between two and three years old, they will start to take an interest in what other children are doing. They may want to join in and will be aware of ideas such as 'sharing' and 'playing together'.
If your child does not do these things, it does not necessarily mean that they are autistic, but it may suggest that they need a little help and support in these areas. Understanding where they might need extra support will make it easier to provide it yourself or to seek professional help.
All children develop and grow in their own time and in their own way, but there are common developmental 'milestones' such as crawling, walking, and talking that generally occur at particular ages. Some children may take longer to reach these milestones, and some may need help getting there.
Use our "Understanding Your Child" checklist to help you understand your child's development. The checklist includes a range of statements relating to speech and communication milestones in children aged two years or older. If you find yourself answering 'no' to most of the statements, you should talk to a speech and language pathologist or your GP. Regardless of how old your child is, it could indicate autism but may also suggest other forms of speech delay.
Click here to download and view the "Understanding your Child" checklist.
How the autism journey begins
In most cases the journey begins by having a conversation wherein you raise your concerns about your child's development with your GP, which leads to them making a referral to the Glenrose Autism Clinic - either the Infant and Preschool Assessment and Outreach Service (IPAS) or the School Age Neurodevelopment Clinic (SNAC)
The journey from first suspecting that your child may be autistic to reaching a diagnosis can be very long - often 12-18 months if a family is accessing the public health system.
Some families opt to have their child assessed at a private clinic to speed up the process. A private assessment can happen rather quickly - in a matter of weeks, but can be rather costly. If you have an extended health plan, your package could cover much of the cost if you have psychology, speech and occupational therapy benefits.
How can an autism assessment be important?
An autism assessment can be important for several reasons, regardless of whether or not it leads to a formal diagnosis of autism. It can give you key information about your child's development and behaviour. It can identify your child's strengths and areas where they may have difficulties. It can also help you to access support for your child's development before they start school and throughout their education.
Assessment during the early years can be beneficial because early support is linked to better outcomes in youth and adult years. An assessment will enable your child to access specific support, including therapy or extra help in school or daycare.
If your child is not diagnosed as autistic, they may have specific difficulties that suggest other conditions such as attention deficit hyperactivity disorder (ADHD), anxiety, attachment disorder, epilepsy, dyslexia, dyspraxia or a wide range of physical health issues. Autism is under an umbrella of wider neurodevelopmental, developmental and learning differences/disabilities. Your child may require further assessments and diagnoses, so this information will still be helpful, as you:
- may be entitled to other forms of support
- can better cater to your child's needs if you know what they are
Taking the first step

If you have a concern that your child is autistic, the first step is a conversation with your GP or pediatrician.
The professional you speak to will have a few questions regarding why you think your child is autistic, or your concern that your child is not meeting the developmental milestones. At this stage, you might feel that, by highlighting your child's struggles, you are being overly negative and ignoring their achievements. Remember that while your child has a wide range of achievements, big and small, the focus of assessments and medical appointments is generally: 'What is wrong and how can I help?'
In order to refer your child for an autism diagnosis, the doctor you speak to needs to understand the cause of your concerns so that they can evaluate whether your child needs an assessment.
To do this, they may ask you what you have observed in terms of your child's behaviour or accomplishments. Since this can be a stressful conversation, and your observations may have happened over a long period of time, it is best to write down all the relevant details in advance. This information will help the doctor get a clear picture of how your child is developing.
How to prepare for that first appointment
Since autistic individuals process things differently, a GP or pediatrician's questions will mainly focus on any signs your child is displaying in relation to:
- verbal and non-verbal communication (including understanding the meaning of common words and phrases, facial expressions or tone of voice)
- relationships and interactions with others, such as making eye contact and knowing how to share
- playing with others and imaginative play - their range of imaginative activities and whether they prefer to play alone or with others.
The GP or pediatrician will want to find out how these compare with the milestones children would commonly be meeting at their age. The doctor may also ask about the pregnancy, your health and whether there is a history of autism in the family
There are a few things you can do to help yourself at this meeting:
- Remember your child relies on you to be their advocate.
- Remember that you have your child's best interest at heart.
- Collect all the relevant information that explains why you have concerns, in writing or by recording videos.
- Take your partner, a family member or a friend with you for support.
What to bring to the appointment:
- your list of your documented concerns
- any videos you've recorded
- any medical records or documents from previous appointments
GP or pediatrician appointments are usually very short and there is probably a lot you will want to discuss. It might be useful to book a double appointment, if possible, to make sure you have enough time to talk about your concerns.
Whoever you speak to may say that you should wait and see; that your child is still growing and developing and may grow out of things you've noticed. They could be right, as all children develop differently. As a parent, however, trust your instincts. If you don't think that sounds right, speak to someone else who knows your child or knows about autism. If your instincts are telling you that there is cause for concern with your child's development and your doctor is not on the same page as you, you may need to seek out a different doctor or seek out a private assessment if you have the financial means to do so.
Assessment and diagnostic appointments
A referral may lead to an assessment and, eventually, an appointment for a formal diagnosis. Receiving a formal diagnosis can bring with it a variety of feelings, from relief to anxiety and everything in between. The most important thing is to remind yourself that these appointments are a step forward.
An assessment appointment may be the first time your child will have been required to be present.
The team of professionals doing the assessment will probably have allowed a set amount of time for the appointment and it is likely that there will be another family coming in after you. But don't be rushed. Make sure you say everything you want to say and ask the questions you want to ask.
What to bring to the appointment:
- your list of documented concerns
- any videos you've recorded - the autism team may prefer to observe your child directly but it may be helpful to have videos to illustrate some of your concerns or observations.
You may be referred for further assessments, including blood tests where there may be other health concerns, but it is likely that you will be notified of the outcome of the diagnosis at the end of your appointment.
Types of diagnostic assessment
There are multiple tools that might be used during a diagnostic assessment. These generally collect two kinds of information:
- your description of your child's development
- the professional's observation of your child's behaviour
Diagnostic tools help professionals to collect information in a consistent way. Current tools include rating scales with questions the professional uses to score your child, based on their observations, discussions with you and other evidence, such as information provided by your child's nursery.
Some rating scales also include sections for you, or others who know you child well, to complete.
Other tools include: a form of a 'structured' or 'semi-structured' interview in which the professional asks you prepared questions; and tools that look at how your child engages in specific tasks.
Whichever tool is used, the professional conducting the assessment will have received specific training in its use.
Commonly used diagnostic tools include:
- Autism Diagnosis Interview Revised (ADI-R) The ADI-R is a semi-structured interview that looks at social interaction, communication and language, and restricted and repetitive interests and behaviours.
- Autism Diagnostic Observation Schedule (ADOS) The ADOS is a semi-structured tool assessing social interaction, communication, play and imaginative use of materials. It consists of a number of tasks in which the professional will seek to engage your child and then to observe how they respond and interact.
- Childhood Autism Rating Scale-2 (CARS-2) The CARS-2 consists of 15 categories that assess a wide range of areas, including relationships, emotions, play, communication and the senses.
- Diagnostic Interview for Social and Communication Disorders (DISCO) The DISCO is a semi-structured interview that assesses social interaction, social communication and imagination, and repetitive behaviours associated with autism.
- Gilliam Autism Rating Scale-3 (GARS-3) The GARS-3 assesses restricted and repetitive behaviours, social interaction, social communication, emotional responses, cognitive style (the way your child thinks and how they process and experience the world) and speech.
A single tool is not enough in itself to provide a diagnosis of autism. Rather, it is used along with information from other sources, such as discussions with you, to help the professional come to a conclusion about your child's diagnosis.
Types of therapy
If other assessments have already been done, you may be offered therapeutic support for your child during the wait for an autism assessment as well as after a diagnosis. The two therapies you are most likely to encounter are speech and language therapy and occupational therapy.
Speech and language therapy
Autistic children interact and communicate differently. They may find it difficult to communicate using words or to listen to and understand what people say. They may have difficulties understanding the non-verbal rules of communication. They may find it difficult to read emotions or understand when to speak and when to listen.
Speech and language therapists work with you to:
- plan practical ways to make communication easier for you and your child.
- identify and plan strategies to support your child to communicate their thoughts, needs and feelings
- help you to implement techniques and strategies to develop your child's attention, interaction and play skills.
Occupational therapy
Because autistic children experience the world in a unique way, they may use their body in a variety of ways to understand how different things feel: they may spin around, rock back and forth, touch things, smell objects or place lots of things in their mouths. They may also get easily overwhelmed by busy environments and run away or hide to escape unfamiliar places that to them seem scary.
These reactions could mean that your child may be trying to communicate something to you, or they might be trying their best to cope with a situation or difficult environment.
Occupational therapists work with you to identify these traits and develop solutions to make daily life easier for you and your child. This might include:
- helping you to plan and implement routine
- helping you develop and implement strategies to make transitions easier, so that your child can cope with moving from one activity to another
- improving your child's independence and participation in everyday activities
- recommending appropriate calming activities that you can easily do at home.
Other therapeutic support
There are other types of support that are available that you could seek out privately or that may be covered under your contract if you have one with Family Support for Children with Disabilities (FSCD). Some people choose private therapy because they may be frustrated with the long wait for an assessment and diagnosis or the long wait to be approved for a contract with FSCD.
When seeking out private therapies, it is important to remember that there is no cure for autism, so claims about cures are false and some of the products and activities that you might find could be harmful to your child.You, your Family & Autism
When professionals talk about autistic children, developmental delays or special educational needs, they often refer to them as having 'additional needs'.
In many ways, as a parent of an autistic child you also have additional needs. As well as bringing up a family, you have to learn about autism, navigate a 'system', be an advocate for your child, and deal with your emotions and those of the people close to you. There is a lot to do and a lot to think about.
In this section of the toolkit, we cover areas such as looking after yourself, supporting your family and looking at ways in which you can be the best help for your child whatever stage you are at - whether you are waiting for an assessment or have had a formal diagnosis.
10 tips for parents
- Be informed about autism, but focus on your child's need and not the label. There is a lot of information out there and it's easy to become overwhelmed. But, every autistic child is different. So, focus on what you need to do to support your child and their needs at each stage of their journey, and take it one step at a time.
- Your child has their own unique personality just like every other child. Love your child for who they are. And don't think that they don't love you, even though they may not say it or ask for cuddles. You are the centre of their universe.
- Don't push your feelings away. Talk about them. You may feel angry or overwhelmed. You may find yourself worrying about a future that is still years away. These thoughts are normal and it's okay to tell people that this is how you feel. No one is judging you - and people around you probably understand more than you think.
- If you feel angry, be angry with the situation or the challenges you and your child face. It doesn't help to be angry with your loved ones. If you find yourself arguing with your family over an autism related issue, remember that the issue might be a difficult one for them too.
- Remember that you have a life too. Don't let autism consume every waking hour. Make time for yourself. Spend quality time with your other loved ones and try not to be constantly talking about autism. Everyone in your family - including you - deserves to be valued, noticed and happy, despite the challenges you may be facing.
- Appreciate all your child's victories, no matter how small. Focus on what they can do. Work with your child's strengths and accept their special interests. Try not to make comparisons with other children.
- You're not alone. Make friends with other parents who have children with autism and who understand your day-to-day challenges and the feelings you experience. Try to build a community of supportive and understanding people.
- Take advantage of all the services and activities for autistic children available to you and your child. Accessing autism friendly services is an easy way to surround you and your child with people going through similar things, and those who are more understanding of your situation.
- Consider integrating your child early on by attending 'mainstream' services and activities. Don't be put off if your child is the only autistic child there. It is not up to your child to 'fit in'; it should be up to the activity to accommodate your child.
- Get involved. Being a champion for autism can be empowering and productive. You may feel frustrated by a lack of support or other people's attitudes. Use that energy to bring about the change you want to see.
Looking after yourself
Your journey is likely to be a long one and the build-up to a child's diagnosis is something you have most likely been anticipating for quite a while. Nevertheless, it is a momentous event. Over the course of the journey there will be times when you need to take stock of your emotions and adjust to the possibility, or the confirmation, that your child has a lifelong condition.
Some people might very quickly see the positives about a diagnosis and will feel positive and hopeful. Some people may take longer to get there. In the next section, Clinical Psychologist Giulia Maccarini reflects on dealing with difficult emotions.
Some thoughts on resilience and self-care
by Giulia Maccarini BA Psychology, MSc Neuroscience, Autism SpecialistEvery stage of the journey can feel hard. All the steps from referral to diagnosis can be full of doubts. You may experience periods of uncertainty and anxiety. And getting an official diagnosis can be extremely hard; learning that your child is autistic will affect not just them but your entire family and those close to you. Right from the beginning your role as a parent/carer will change and that can lead to a range of emotions and reactions. However you are feeling right now, it can help to remember that getting an early assessment will enable your child to receive early intervention.

To some parents the prospect of autism is a shock. To others it is the confirmation they needed, while still others experience denial. It is important to understand that all of these feelings - including denial - are valid.
Parents-to-be often idealise their child from the moment they find out they are having a baby, some even before that. They imagine what they will look like, what characteristics they will inherit, what their likes and dislikes will be, whether they will have friends, learn other languages, or travel the world.
Some parents of autistic children have described feeling as though everything they had hoped for and imagined for their child had been taken away. For some parents, the process might trigger a sense of grief; a feeling that they have lost the child they dreamed of and that another child has been given to them. This sense of grief can come with a range of other feelings.
You might feel sad. And feeling sad is normal. Allowing yourself to feel sad can help you to grow and understand. You might also feel angry, and anger is also a natural part of the process. Expressing those feelings is a healthy way to better understand yourself and how autism impacts you as an individual and as a parent.
The journey through autism in the early years can also feel very lonely, especially since parents can have different reactions. A couple raising a child together can have different views and feelings around the diagnosis. Having different perspectives can make you feel isolated from one another and overwhelmed. Don't deny or ignore your feelings. Anger, sadness and loneliness are all part of the path to acceptance and part of what will make you more resilient.
Build your resilience
Resilience is defined as 'the capacity to recover quickly from difficulties'. The act of building resilience comes from focusing on your feelings, practising acceptance and learning to get up when you fall. It's important to shift your focus from thinking to doing. In times of adversity there is nothing to be gained by feelings of blame or regret. Focus instead on what you have to do; having a purpose can motivate you to persevere through the process before and after diagnosis.
Build a network
Having a network of people who understand and support you will help increase your resilience. Knowing that you are not alone, and being brave enough to ask those around you for help, is a more efficient use of your energies and can motivate you to persevere despite the hardships.
Take care of yourself
Caring for an autistic child can be both emotionally and physically draining. Finding space to care for your own personal needs is not easy, and might take time, but is vital for your health. If you've ever travelled by plane, you will have heard the safety instructions at least once: 'Put on your own oxygen mask first, before helping others.' You need to follow the same principle; you can't help anyone else without helping yourself first. It often doesn't take much - sometimes just going for a walk will give you the space to breathe so you can begin to feel like yourself again.
Focus on the positive
When difficult days happen, we tend to focus solely on what made it hard and we rarely reflect on the positive things we've achieved or that also happened during the day. Today might not have been the best but make a point of identifying the good things and celebrating the positives. Write a short list of what was good that day. You'll be surprised by what you find.
Give yourself time
You don't need to strive for acceptance straight away. It's OK to have negative feelings towards a possible or confirmed diagnosis. Difficult emotions can't, and shouldn't, be buried. These thoughts will always try to get in and they are likely to be persistent. But, in the same way we can choose not to answer a ringing phone, we can - with practice - choose not to let certain thoughts take hold.
Be realistic
There's no perfect mother or father, but every parent is doing what they can to help their child.
Explore interests outside of the autism world
Keep in mind that you are more than just a parent of an autistic child. Exercise, go out for a meal, read a book, watch a movie or take up a hobby. Look after yourself so that you can look after your child.
Ask for help
If you have trouble working through your feelings and emotions, seek the help of your partner, your parents, your friends, your GP, a support group, a psychologist or a professional in counselling. There is no shame in asking for help to cope.
A final thought. There is a popular folktale in which a group of a wise advisers tell a king that, whatever problems, or triumphs he faces, he should always remember that 'this too shall pass'. It's true. Bad moments will pass, and good moments will too. The uncertainty, the difficult moments, the much-celebrated victories - all will come and go. Events and emotions are like waves. We can't stop them from coming, but they always roll over us and, just as in the king's story, they too shall pass.
Talking to your family and friends about your child's needs
Telling your family and friends that your child may be autistic can be difficult. Some family members might dismiss your concerns, suggesting 'they'll just grow out of it', or that your child's behaviours and actions are something to do with the way you parent. Some family and friends will be incredibly supportive and will want to know what they can do to help. Reactions can vary widely, but it's important to share.
It might help to keep people informed about where you are on the journey. You could start by explaining that although your child may not have had an assessment or diagnosis yet, you and the professionals that you have spoken to are concerned about your child's development and feel it's important to check things out. It can be helpful to explain what you have been through - how you (or someone else) became concerned, that you spoke about it with your GP or another professional, and that they suggested a referral for an assessment.
Talking about a possible diagnosis of autism might help your family and friends to understand that there is a reason for some of your child's behaviours. They may even have noticed some of these behaviours already; for instance, that your child only likes to play with one thing, doesn't speak or doesn't like certain textures or sensations.
Educate your family and friends. Tell them about what you've learned:
- Autism is a spectrum with varying degrees of complexity.
- Autistic children often have difficulties with their communication and their ability to interact with others, and may have restricted or repetitive patterns of behaviour.
- Autistic children can have highly developed skills and abilities.
- You are seeking an assessment to provide you with important information about your child's behaviour and development.
If those around you understand why your child displays these behaviours, they might stop worrying about them, or having unhelpful opinions about them, and begin to accept and work with them.
You should be prepared for people who won't, or can't, understand or accept what is happening. Some friends and family members may say that you are being overcautious or that your child's development is just a bit delayed. This may simply be the view of someone who doesn't live with your child on a day-to-day basis. It may take them longer to come to terms with what you are telling them about your child.
If someone from a health team or your child's school or daycare has suggested some tips or strategies to support your child's development, consider sharing these with your family and friends. You can achieve more if everyone is working towards the same goals.
Involving your family and friends
Everyone around you can help you to support your child. Encourage your friends and family members to learn about autism and keep believing in what you are doing. Despite any differences you may have, try to focus on the love you all share for your child.
To help you to start a conversation with your family and friends and suggest ways in which they can help and support you.
If your child has siblings, it is important that they feel involved and informed.
9 tips for grandparents and other family members
- Ask how you can help your family as they support your loved one with autism. Every family member has something to offer, and your efforts are bound to be appreciated. Showing support can come in many ways, whether it's looking after the child for an hour so that their parents can have some free time, helping to find local support services, or even helping to fundraise for your loved one's school or daycare.
- Learn more about autism and how it impacts your loved one. Around one in 44 people are autistic and it impacts every one of them differently. It may be a life long condition but it isn't a life sentence. A young autistic child has a rich and promising life and, as they grow, you will learn their likes and dislikes, their talents, and their challenges - just like any child. Share that sense of hope with your family.
- Look for support for yourself. If you find it difficult accepting and dealing with the fact that your loved one is autistic, seek out your own support. Your family members are dealing with their own emotions, so they may not be able to provide you with support. Find a trusted person outside of your family to talk to.
- Be open and honest about autism. It may be hard to talk about it at first but, as time goes on and as you learn more about autism and your feelings about it, it will be easier.
- Try not to compare your loved one to other children. All children develop at their own rate and each child has their own strengths and gifts.
- Make special time for every child in the family. You can enjoy special moments with family members who develop typically and those with autism. They all enjoy spending time with you.
- Autistic children thrive on routines. Find something that you can do together that is regular and structured, or is linked to something the child is particularly interested in. Even if it's just watching the trains in the station or doing a jigsaw.
- Focus on your loved one's needs and not the label. There is a lot of information out there about autism and it's easy to become overwhelmed with it all. Every autistic child is different. Focus on what you need to do to help support the autistic child in your life at each stage of their journey, and take it one step at a time.
- Learn how to be an advocate for your loved one with autism. Learn how to stand up for them, how to educate other people, and how to love them for who they are. Understand that people are often fearful of things they don't know or don't understand, and that judgement comes from ignorance. You have the opportunity to share your knowledge and to help others feel more understanding of, and more comfortable with, all autistic people.
Tips for brothers and sisters
- Be proud of your brother or sister. There's no reason not to be open when you're talking to your friends about autism, and there is no reason to be embarrassed of your sibling. Your sibling thinks a little different than you do and that should be celebrated!
- Love your brother or sister for who they are. You would want them to do the same for you. Try to highlight what your sibling is good at; we all want to be recognized for our strengths.
- Even though you love your brother or sister, sometimes you may feel as though you do not like them. That's okay - all brothers and sisters feel like that at times and this is a completely normal emotion to feel.
- If you're finding it too much, make sure you tell someone. Don't bottle up your feelings. If you feel you can't talk to your parents about it, try finding someone else who will listen. There are other people you can talk to who care about you, like your teacher or other family members.
- Remember your parents may be struggling too. Try not to take it out on them. Sometimes life can be hard, and everyone is trying to do their best.
- You are not alone! There are tons of families who have autistic children, parents, and even grandparents! This is amazing and we are certain you will come across many siblings of autistic individuals in your life.
- Learn about autism so that you can become comfortable talking about your sibling with friends and classmates. Explaining autism to others means that more people will become accepting of people who learn differently, and that's good for everyone.
- It's okay for you to want time alone. Having an autistic sibling can be tiring and frustrating. Sometimes it helps just to have a bit of space.
- Find something that you and your brother or sister enjoy doing together. You will find it rewarding to connect with them, even if it's just a simple thing like doing a jigsaw puzzle. What's boring to you might be really exciting to your brother or sister. So, just join in. They'll be so happy they can share that with you.
Supporting your Child
Whether you are at the referral stage or have a diagnosis, you are still your child's primary carer and their first teacher.
Many of the challenges that parents or carers of young children face, such as weaning or getting a child into a sleep routine, are often more challenging when your child has additional needs or a disability. Many parents of autistic children report that the areas that they most want help with are:
- Sleep
- Eating
- Toileting
- Behavior
There are people and services who can help with these challenges. You can look for an Occupational Therapist with experience with these challenges and support may be available through your FSCD contract.
What you can do to help your child's communication
Many of the characteristics of autism relate to communication difficulties, so it is important to support your child's communication development. Here are 10 tips to help you.
- Follow their lead. Follow your child's lead, rather than directing them. They will be more likely to pay attention to the activity and focus on the same thing as you if they are interested and motivated to begin with.
- Be face to face. Face your child and get down to their eye level when communicating so that they can see the variety of facial expressions used in communication.
- Copying. Copy your child's actions and sounds. If they use a sound like 'vroom' instead of 'car', don't correct them - just go with 'vroom', because you both know what they mean. If they bang the spoon on the table, and you do the same, it is likely that they will pay attention to you. This can help your child begin to understand the power of communication.
- Get involved. For example, if your child is lining up their cars in a row, join in by handing them cars one by one. If they are only interested in throwing the toys on the floor, you could use a basket to collect them before giving them back. Show your child that you're interested in the same things as them and that interaction can be rewarding and interesting too.
- 'High-interest' objects. Blowing up a balloon and then letting it go so that it flies up in the air usually gets a child's attention. Blowing bubbles often has the same effect. If things like balloons and bubbles get your child's attention, then use them to encourage two-way communication. Blow up the balloon part-way and wait for a response before blowing it up to its full capacity. Blow a few bubbles, then close the container and wait for a response from your child before you blow any more. Don't continue if your child reacts badly, just try a different 'high-interest' object that will get their attention in a positive way.
- Encourage requests. Place favourite toys or foods somewhere slightly out of reach, on a shelf, for example, where your child can see it but is unable to reach it. Alternatively, place the favourite object in a container that is difficult to open, such as a plastic container. This will encourage your child to ask for help and result in an interaction.
- Give them things gradually. For example, if your child wants a cookie, you could break it into small pieces. Start by giving them one piece and then gradually give them more once they have communicated a request for it.
- The words you use - 'less is more'. If your child does not yet talk much or at all, then build up the use of words gradually. For example, if your child just uses the name of a toy they reach for, just add one more piece of information to what they say. For example, if they say 'car', you can reply 'yes, blue car'.
- Use gestures and visual supports. When offering a drink, mime the action of drinking. Nod or shake your head for 'yes' and 'no'. Wave your hand for 'hello' and 'goodbye'. When talking about people - for example, 'Grandma is staying' - show a photo of who is being spoken about. When you go out, show a photo of where you are going.
- Most of all - have fun playing together! Don't force any of these things. If they're causing distress then stop. Use these tips as a starting point to find what works for you and your child.
Supporting your child's play
All young children enjoy and benefit from play. Autistic children are no different. But play is more than just fun. It is very important developmentally. It is the way in which every child explores the world and makes sense of it as they grow and learn. Play also helps children to develop important physical and social skills.
Sometimes, play can look different in young children who are autistic. They may be interested in only a very small range of toys - possibly only one or two - or they might do the same thing over and over. Your child might not use toys in the way you would expect them to. For example, they may be interested only in spinning the wheels on a toy car rather than pushing it along the floor.
Autism can affect the development of social skills and communication skills. Play provides a useful opportunity to help nurture and develop some of these skills. By helping your child to play, you can also help them to develop their imaginations, as well as their social and communication skills. For example, they can learn about taking turns, asking for help and making choices.
Below are the six main types of play, with specific suggestions for helping your child:
Exploratory play: learning about the world and your body by exploring different textures, shapes, and sizes.
You can help your child's exploratory play by joining in and encouraging them to explore a wide range of shapes, textures, and sensations, including water, sand or foam.
Interactive play: playing with toys that require your child to do something such as press a button, to make something happen.
Your child may work out how to use the toy themselves or you may need to help by showing them. Either way, be sure to praise your child when they get it right, and encourage them to explore other toys that use the same cause-and-effect principle. This will help them to understand that their actions have effects and give them a sense of control in their play.
Cause-and-effect toys are also a good way to teach your child how to ask for help and to play by taking turns. For example, you could take turns pressing a button to make something pop up and then take turns pushing it back down again. To help communicate these ideas, say simple things like 'Mommy help' or 'Daddy's turn'.
Toy play: playing with toys as they were designed to be used, for example throwing a ball or pushing a toy car.
Try not to overwhelm your child with too many choices. Offer two or three toys at a time and let them choose which one to play with.
Join in with your child. Sit in front of them so that you can watch each other use the toy. Join in the play, rather than instructing your child. Begin by copying what they do with the toy, then ask for your turn and introduce a new action. If your child likes squeezing a ball, do the same but throw it in the air or roll it towards you before squeezing it.
If your child doesn't copy you, encourage them by saying, 'Your turn to roll the ball.' Or guide your child's hand in the rolling action.
Use frequent praise in clear language. For example, say, 'Good throw. The ball went a long way!' You can use rewards such as blowing bubbles or something else that your child enjoys.
Look out for signs that you child is losing interest or getting frustrated. Before this happens, try to end on a positive note, with your child having accomplished something.
Constructive play: building or making things - such as building a tower out of bricks, drawing a picture, or completing a jigsaw puzzle.
Start by showing your child what to do. If your child struggles with a task, break it down into smaller tasks. For example, if your child is struggling to complete a jigsaw, you could encourage them just to do the final piece, before gradually introducing more pieces to complete the jigsaw. That way, things stay more positive because your child always succeeds.
Start with simpler tasks and make them more challenging as your child's skills develop, such as jigsaws with more pieces, or using smaller bricks for a tower.
Physical play: physical activities such as running, jumping, or dancing that use the whole body help your child build muscle and improve coordination.
Physical play gives children the experience of interacting with other people and objects in their surroundings. Playing outside gives your child the chance to explore the natural environment, have adventures, discover their physical limits, and build self-confidence.
When your child is outside, they probably have more space and freedom for big movements, like running, jumping, kicking, and throwing. Such activities are good for your child's health, fitness, and physical development. Outdoor play can also mean more mess - and more mess often means more fun.
Pretend play: pretending and using your imagination during play. Examples include dressing up or pretending to have a picnic with dolls and teddy bears.
Using their imagination during play helps your child develop language, communication, and social skills. This type of play is often delayed in autistic children, but many children can and ultimately do develop pretend play.
Social play skills for children with autism
Social play skills usually develop and evolve gradually from playing alone (solitary play) through to playing and cooperating with others. The ability to play with others can be particularly challenging for autistic children.
The four key stages of social play were developed by American sociologist Mildred Parton Newhall in the 1920s and are still widely used to describe children's progression through different and more complex types of play. Whatever stage your child is at, there are things you can do to help them move on to the next stage:
Solitary play: when your child is alone and is playing independently. Whatever stage your child is at, they're likely to want to spend time playing by themselves. It's OK if your child wants to play alone some of the time.
Parallel play: when children play alongside each other, often separately from other children but perhaps watching them or mimicking their actions. This type of play is seen as a transition stage to more social and cooperative play. You can help to promote parallel play by encouraging your child to play alongside other children, including siblings and cousins, or through 'play dates'.
Associative play (playing and sharing with others): the stage at which children begin to interact with other children, often through sharing, taking turns or coming up with ideas or suggestions. Encourage your child to begin incorporating these things - for example by encouraging them to swap toys or do something similar to another child, such as ride a bike if the other child is using a scooter.
Cooperative play: involves games and activities such as hide-and- seek where there might be rules or when you need to work together to make something like a fort or a sandcastle.
Cooperative play can be complicated and usually involves communication skills. The social rules involved in this type of play can be difficult for children with autism. You can help your child by using clear and simple instructions. For example, you could say something like: 'First, you hide somewhere in the garden. Then Jo counts to 10. Then Jo comes to find you. When Jo finds you, it will be your turn to count to 10 while Jo hides. Then you have to find Jo.'
It can also help to explain the rules of the game using visual support such as pictures or 'social stories'. Making games more visual can also help. If you are organizing a game of tag, for example, you can mark the person who is to be chased with a scarf or a piece of cloth.
Making the most of play
Play is a useful tool to help you build skills in other areas. For example, you might focus on communication skills by asking your child to describe what is going on in the game or encouraging them to choose what to do next. You can use play to develop social skills such as taking turns by offering praise and simple rewards.
Here are some tips for using play in this way:
- Talk about what's happening while your child plays. Use the names of objects, like 'car', 'ball' and 'paint brush'. Gradually add single words such as 'blue' to 'car' and 'big' to 'ball'. You can also give words to the things your child is doing, for example 'feed teddy'. Over time, you can build longer sentences.
- Use play to help your child settle into new environments. For example, if your child likes building towers with blocks, encourage them to build a tower with other children at a friend's house.
- Use play to support everyday routines such as bath time.
- Opportunities for play happen all the time. If your child is interested in an object that they see, use it to create a game, for example 'find the hairbrush'.
- Use play to help your child cope with social rules or situations that they might find challenging. For example, hold a birthday party with teddy bears and dolls to explain what will happen when your child is preparing to go to a friend's birthday party.
- Use play to help your child develop everyday skills. For example, dressing a doll or changing in and out of dressing-up costumes can help your child learn to dress themselves.
- Use play as an opportunity for you and your child to have fun together.
Going out and about with your child
There is often still a lack of awareness about autism in society. This can lead to uninformed people misjudging autism as 'naughty behaviour'. This in turn can have a big impact on your emotions if your child begins to struggle in a public place.
As a parent, you may feel a range of difficult emotions such as shame, guilt, anger, and helplessness, if you're out in public with your child and they are struggling to cope. It can be difficult to feel like a good parent if your child is having a meltdown due to sensory overload, or 'stimming' to self-regulate and soothe themselves. It's harder still if you feel like others are judging you.
People may be better able to understand your child, and how they can help, if you share information about them.
Your child has the right to be integrated into the community and to experience life outside the house, even if their actions and behaviours look different.
One-page profile
How to use 'My one-page profile'- My diagnoses Use this space if your child has a formal diagnosis. Briefly describe the outcome of the diagnosis. List all the conditions, such as epilepsy, speech disorder, and so on. If you don't have a diagnosis yet, use this space to describe your situation, for example: 'I have been referred for an assessment' or 'I am receiving speech and language therapy'.
- My medication Describe what medicines your child needs and when and how they are administered, for example: only by you, when needed or by agreement with you. Leave blank or write 'none' if your child does not need any medication.
- My allergies Leave blank or write 'none' if your child does not have any allergies. If there are foods they really don't like or react badly to, use the 'Things I don't like' box to describe them.
- How I like to play Use simple phrases, for example: 'I like to play on my own', 'I like to play in small groups' or 'I like toy cars/cuddly toys', and so on. Also use this space to describe how your child likes to be with other children. Be honest but be positive, for example: 'I like to play with other children but find it hard to share sometimes'.
- How I talk and communicate Describe your child's language. For example: 'I don't use many words' or 'I understand instructions better if you point or use pictures'.
- Things I like This could include special interests, friends, certain clothes, being cuddled or being left alone, or actions such as flapping, dancing, running, humming, and so on.
- Things I don't like This could include sensory stimuli such as bright lights and loud noises. It could also relate to communication-related issues such as direct eye contact.
- Things that help when I'm upset Use this space to describe the things your child might need in order to be soothed or the things they do to soothe themselves. This may be things like having a favourite toy or comforter, or getting a cuddle.
- Things that show I'm upset Use this space to describe the kinds of behaviour your child starts to display if they get agitated or upset. These might include covering their ears, making noises or repetitive movements.
- Things I'm good at Use this space to describe your child's strengths, talents and abilities. Ask your child what they'd like to say in this box.
- Physical prompts. Going to visit a new location - such as a doctor's office or hairdressers - before an event so your child is physically familiar with the environment.
- Make back-up plans. Sometimes you may have to consider additional planning for special events such as birthday parties or when you're in large public spaces, for example a football stadium or busy swimming pool, where things might change unexpectedly. Having a back-up plan can be really helpful. Is there a quick exit if your child becomes distressed? Will it be loud? Would ear defenders help? Does your child have a favourite toy, game or book to occupy them during any unexpected, unstructured time?
- Look out for patterns to help you work out the cause of your child's behaviour. For example, a parent we spoke to told us that her son would resist going into some new places but would happily go into others. Eventually, she worked out that he didn't like going through a closed door. So, some shops were OK, as their doors were always open or would open automatically, but he would get anxious if the door was closed. Going ahead of him and opening the door helped solve the problem.
- what is going to happen
- the past and the future
- their feelings and the feelings of others
- how to do things independently
- what they need to know about difficult situations
- the choices available to them
- Place a symbol, drawing, photograph or image on each side of the board.
- Show your child the board, point to each symbol and reinforce the message with simple instructions. Don't use a lot of words. For example, say 'brush teeth now ... put pyjamas on next'.
- When your child has finished with the activity, you should inform them by saying 'brushing finished, pyjamas now' while pointing to the next picture.
- One thing to bear in mind is that you can use the 'Next' side of the board to place an activity that really motivates your child to act. This can work as a reward, something your child can aim for.
- Have a dedicated space for it where your child can see it easily and often (on the fridge door perhaps, at your child's eye level).
- Take the timetable or a copy with you when you are out for the day. Use it to remind your child what they have just done and what will happen next.
- Actively show that an activity has finished by ticking or removing the symbol or picture.
- Review the timetable at the start and end of each day if your child finds this helpful.
- Match the language and vocabulary levels of the child.
- Present it when the child is relaxed and distraction free.
- Use 'social stories' frequently prior to the actual event.
- If possible, ask the child to repeat the story and share it with others.
- Present the story in a simple format, Black ink on white paper works well but some children find coloured paper easier to use.
- Stress the steps that you know are going to be the tricky ones. For example: 'There will be a long queue and [use your child's name] will need to wait.'
- Use rewards at the end of the event. For example: 'If you sit in the shopping cart so that Mom can buy five things, then Mom and [your child's name] will go to the toy section to see and touch toys.' Don't be afraid not to give the reward if the steps are not followed. I had to do this only a couple of times for my son to realize that I was serious when I said that the reward would only be given if the steps were followed.
- Know your goal. Be clear and specific about what you want to achieve and focus your story on that goal. It could be as simple as 'now' and 'next': 'Now we brush our teeth. Next we get into our pyjamas.'
- The beginning, the middle and the end. A successful 'social story' just needs three things: a title and introduction that clearly identifies the topic; a body that adds detail; and a conclusion that reinforces and summarises the information. One or two stick figure sketches will help illustrate what you are talking about and can be used as a visual reminder while the event or activity is going on.
- Keep it brief, keep it simple. Try to tailor the story you have drawn and are describing to match the language skills, attention span and interests of your child.
- Sound positive. Describe everything in a positive and patient tone.
- Who is in the story? You might want to use either second- or third- person language, for example: 'You will then go to the shop' or 'Suzi will go to the shop'. You might need to experiment to find out which one your child responds to best.
- When does the story happen? Be consistent when using past, present and/or future tenses. Don't jump from one to the other in the same story. For example, try not to say: 'The last time we went to the pool the water was cold. When we go tomorrow, it will still be cold.' Instead, create a story that helps your child to remember the last visit to the swimming pool, or assume that you've never been before and describe how it will be. Once again, experiment to see what works best.
- Who, what, when, why, where and how? Try to incorporate the full range of 'who, what, when, why, where and how?' You don't need to draw these; just explain them as you go, pointing at the pictures you have drawn. When it comes to 'why', you should think about explaining the basic rationale behind the event or activity.
- Describe rather than direct. A 'social story' is based on descriptions rather than direction: 'the music at the party will be loud' rather than 'there will be loud music at the party so find a quiet space to go to'. You might want to use 'coaching sentences' at this point, such as: 'The music will be loud. That's because some children like that and it makes them want to dance. It's OK if you don't want to dance.'
- Practice makes improvement. The old proverb, 'if at first you don't succeed, try again', applies perfectly to 'social stories'. This may be new to you and your child and it might take a few attempts for you to both feel comfortable with it. If it doesn't work first time, that doesn't mean it won't work at all.
- Praise your child. When you praise your child at the end of the event or activity, remind them about the 'social story' you used and how everything you talked about happened and how much better things were because you had both been able to 'rehearse' what was going to happen. This will build your childs trust and confidence in you
Click here to download and view the One-Page Profile.
Preparing for situations outside the home
While it's true that certain locations or events might prove challenging for your child, there are things that can help both of you to prepare for these situations and to conquer life outside the home. These include:
Your child might feel more secure and less anxious if they already know what to expect at a new event or in an unfamiliar setting. A simple and useful technique to prepare your child for what will happen, and who will be involved, is to use visual support. The next section covers what visual support is and how to use it.
Visual support
Consistency and routine are important to autistic children. The world can be a very unpredictable place for young children on the spectrum and this can be frightening and can create anxiety. Knowing what is going to happen, and when, can help young children to manage this anxiety.
Visual support is about using pictures or real objects to help your child understand what is happening or anticipate what is going to happen. At its simplest, you can use real objects, for example: show your child a cup when asking if they'd like a drink; or photographs, pictures on your phone, line drawings or symbols if you're talking about going to a shop or someone visiting your home.
Using visual support gives your child another way to communicate while their speech is developing. Visual support can help your child understand:
There are several methods of using visual support, including Now and Next boards, Time Timers, visual timetables and 'social stories'.
Now and Next boards
Now and Next boards are a simple visual support to help a child move from one activity to another. There are two columns - one for 'Now' and one for 'Next', with space for you to draw a simple picture or symbol or stick a photo or image under each.
How does it work?
Time Timers
The concept of time can be very difficult for any child to understand. When you say 'five more minutes', a child has no way of knowing what that really means. A Time Timer is a commercially available type of clock designed to show the passage of time. As the time ticks down and the red disk gradually disappears, your child can clearly see the passing of time, have a better idea of how much time they have left and know clearly when something has finished.
For example, if you use the Time Timer to tell your child they can watch TV for 10 minutes, you could say, 'So, when the red stops moving and the beep sounds, TV time is finished.' This provides both a clear instruction and a way to help your child 'visualize' the amount of time they have and when the activity is meant to finish. It helps them anticipate that the activity is coming to an end and provides them with a concrete 'finish time'.
Time Timers can be used in a variety of situations, including to support your child when they are brushing their teeth, having a bath or playing with a particular toy.
This can be helpful in supporting your child to transition from one activity to the next. Using a Time Timer also promotes positive routines and can help your child's self-regulation skills, as they are less likely to be upset if an activity suddenly has to stop.
Visual timetables
These work a little like a Now and Next board, but cover longer sequences of activities. A timetable can be created for the day, for the week or even the year if you have a particular event, like a holiday, that you need to prepare your child for. A visual schedule, using pictures and symbols, helps your child to know what is going to happen and can help with the transition from one activity to another: 'Today we are going to drive to the supermarket to buy food. We will then drive to Grandma's. We will then have lunch. We will then drive home. You can then play. We will have our snack...' - and so on.
Be guided by your child's needs and preferences; some children find it reassuring to see the whole day at once, while others find that overwhelming. At first, it may be helpful to 'start small', with a few activities at a time, and then to gradually extend the length of the sequence you use as you and your child become familiar with the system.
If you are using a visual timetable:
Social Stories
Social Stories are another form of visual support. They were created in the 1980s by Carol Gray, a teacher in the USA working with children with special needs. Carol had observed that many of her pupils struggled with unpredictability. She began sketching out storyboards for her autistic students that broke down a complex chain of events into simple steps that could be explained and rehearsed.
To find out more about Carol Gray and Social Stories, visit https://carolgraysocialstories.com/
A parent's experience
The best way to describe how visual support works, how these techniques are used and how they may benefit you is through a parent's experience. On the next page, a parent shares her experience of using visual support with her autistic child.
What's the big deal about social stories?
by Manaz Pimple, parentOur story started when our son was two years old, and we began to suspect that something was not right. After all the usual appointments and waiting lists, he got his diagnosis of autism at the age of five.
The period between knowing that something is not right and then receiving the formal diagnosis is a very difficult period for us parents, as we don't receive much support or information on how to interact with and help our child. For the child this is a very critical period as well because, at this age, they are beginning to learn to build trust, establish relationships and develop a sense of the complicated social aspects of our human behaviour that we take for granted.
My son was three years old when I was introduced to the concept of 'social stories' by a speech and language therapist. My first reaction was to laugh it off. I remember telling her: “He barely has any speech, he can't sit in one place for more than two minutes, I don't know what his language comprehension skills are, and you want me to show him images and tell him stories. How is that going to help with his meltdowns? How is it going to help me manage his behaviour once we are out of the house?”

Her explanation has stuck in my mind forever: “When you leave the house to go shopping, you know in your head when you are going, which shop you will go to, how you get there, what exactly you want to buy and what time you are coming back home. An autistic mind needs this confirmation 10 times more than your mind. They need to know the 'what next' at all times. If they don't, then the sensation of anxiety begins to build: 'What is going to happen next? Am I going to fall in a black hole!' This heightened anxiety then puts their nervous system into the 'fight or flight' mode and that's when you have meltdowns, sensory overload, and other behaviour problems.”
Then came my next concern - I don't have the tools or time to create social stories for every situation. I don't have easy access to a computer or a printer, or the time to search for images. To these concerns, she replied: “Can you draw? I am sure you can draw stick figures. All you need is a pencil and a notebook.” I had no more excuses then! So began my first experience of creating 'social stories' and experiencing the magic that followed.
The first time I put it to the test was when I was travelling with my son all by myself. Airports were particularly tricky. He did not like waiting in the queues, he would have a meltdown when they would take his favourite toy and put it on the scanning belt, and he would refuse to sit down in the waiting area. On the plane he would keep standing on the seat, saying “home, home” every half an hour and crying. I would just wait for him to fall asleep. So, on this particular journey I tried using a 'social story' to explain to him what was going to happen and what was expected of him.
I took him through the story a couple of times before we left. Then, as the situations unfolded, I took him through it again so that he could anticipate what was happening next. It was magic! He waited patiently in the queue and did not cry. Instead, he counted up to 10 with me while his toy went through the scanner and sat in the plane seat and was much calmer throughout the journey.
From then on 'social stories' became my son's crutch. I use the comparison of a crutch because, as a sceptical mum, I quickly began to question what would happen if my son got so used to 'social stories' that he refused to function without them. My speech and language therapist had the answer: “When you break a leg, you use a walking stick or a crutch until your leg heals and you gain the strength and confidence to start walking. It will be the same for your son. Once he gains trust and understanding, and develops his speech, his reliance on 'social stories' will automatically fade away or you will be able to use them in a more casual way.”
I was no longer worried about taking my son out or going to social events. All I had to do was to know what would happen while we were out or at an event, and draw a simple 'social story' to explain the steps and take him through it before the event.
We survived so many tricky situations with the help of 'social stories': eye tests at the hospital, his first haircut, weekly shopping trips and his first day at school. I also started to use 'social stories' to prompt appropriate behaviour.
The things I find important to remember when using visual support are:
The beauty of using visual support was that it helped us work towards building trust. It made my son feel so much more in control. As a result, he was calmer and became more receptive to things changing unexpectedly. All I had to do was say “oops'', change the drawing quickly and show him. Gradually, I moved to just verbally explaining to him what would happen and then, if there was a sudden change, he would just shout out: “Oops, the swimming pool is shut - we will now go to the park.” There were no meltdowns!
I know it is not easy, but it is all about trial and error. 'Social stories' worked for me and I hope they work for you as well. As parents we need to plan a little better and to anticipate things in advance so that we can help our child feel more in control. It is possible.
'Social story' products and systems
Practical Support
AHS Early Intervention Program
A home-based educational and support program for families who have a child, aged birth to 3 1/2 years with two or more developmental delays and / or a diagnosed disability. Provides support, education, and information to families of children with two or more developmental concerns or a diagnosed disability, in many settings and locations; family's home, playgroups, and in the community. Parents should call if they have concerns or questions about their child's:
- Attention
- Movement
- Feeding
- Speech
- Hearing
- Interaction with others
Services to families and their child include:
- visits with you and your child in your home and/or community child and parent groups
- activity ideas to support and build your child's development
- referrals and support in accessing other services and resources
- developmental screening
- resource lending library
- assistance in planning for your child's preschool years
Childcare
Looking for childcare can feel daunting, as you may be preparing to leave your autistic child in someone else's care for the first time. However, good quality childcare is beneficial for all children and will support your child's development, independence, and social skills. Most families choose a daycare close to their home or place of employment, make sure to consider how well the childcare setting can accommodate any additional needs your child has. If an aide is needed to ensure the safety and supervision of the child and to have the child included in activities, FSCD can provide this additional support. Please see the section on FSCD to find out how to apply for this service. Please note that aide services will not be provided by FSCD if the child is eligible to receive the same service from another government department, such as Alberta Education or Alberta Health.
FSCD (Family Support for Children with Disabilities)
The FSCD program is based on the Family Support for Children with Disabilities Act (FSCD Act) and the FSCD Regulation. We work in partnership with eligible families of children with disabilities to help parents:

- with supports and services to raise your child and promote their healthy development
- encourage your child to take part in activities at home and in community
- maintain guardianship, responsibility for decision-making, and usual expenses to raise a child until they are 18 years old
- with some of the extraordinary costs related to your child's disability
Services are tailored to meet your family's situation by working together with you to:
- determine your child and family's specific needs
- set goals to help your child develop and participate at home, school and in the community
- agree on services and resources to help achieve your child and family's goals regularly review your goals and needs
Visit their website for more information: https://www.alberta.ca/fscd.aspx
How to apply for FSCD - visit the My Alberta Supports site and fill out an application online: https://myalbertasupports.alberta.ca/CitizenPortal/application.do
Education
Early Education Support through Program Unit Funding (PUF)
Alberta Education provides funding for preschool-aged children who are 3 or turning 3 by December 31, up to the age of 5, through Program Unit Funding (PUF). PUF is provided from September to June in the child's preschool or daycare setting. This funding provides educational support and a multi-disciplinary team to work on goals which are guided by an Individualized Program Plan (IPP). There are several PUF providers throughout Edmonton and area, and you can choose which style of PUF services best meet your child's needs. Some of the providers have site-based programs which are a classroom setting where all the children in the class will be there because of their funding. There are other agencies that provide PUF services and they bring their supports to the preschool or daycare that your child is already in so that your child is integrated with typically developing peers. PUF spots fill up quickly, so it is best to look into the programs in February and March so that your child can be registered for September when the programs start. You can see a list of PUF providers on our Next Steps Guide
Educational Support in the Classroom
Through the Specialized Learning Support Grant, your child will be able to attend a regular school classroom with support. Your child should receive an Individualized Program Plan and the supports that they require to be successful. You should speak to the administration team at your child's designated school within your school district and work with the team to set up supports for your child.
Education Options
Edmonton Public Schools has an Interactions Program that is available at several schools throughout the district. The Interactions program supports autistic students. Autism can impact how people understand what they see, hear and sense. This lifelong disability can result in difficulties in communication, social relationships, behaviour, or learning. Although some autistic students achieve at grade level, many have uneven or delayed achievement. Please see their website for more information: https://www.epsb.ca/programs/interactions/ Edmonton Catholic School Division has the GIST Program- The Guided Intervention Supported Transition Classroom supports children with Autism Spectrum Disorder (ASD). This program is available at St. Gabriel School. Please see their website for more information: https://www.ecsd.net/8217/page/4866/gist
Individualized Program Plans (IPP) - sometimes called Individualized Service Plan (ISP) or Individualized Education Plan (IEP)
If your child has an autism diagnosis, they will likely receive support through Alberta Education either through Program Unit Funding (PUF) if they are preschool-aged or through the Specialized Learning Support Grant if they are in kindergarten through to Grade 12. If your child is receiving support through Alberta Education, there should be an IPP (or IEP, ISP) in place to guide the teacher and learning team with goals and outcomes for the current school year. The IPP should include any accommodations or supports that will be put in place to help the child or student be successful.
- Assess: Your child's difficulties must be assessed and diagnosed so that the right support can be provided.
- Plan: With your involvement, your child's school or PUF provider will implement an IPP (Individualized Program Plan) intended to work toward specific goals; in other words, how your child will benefit from any support they get. All those involved should have a say in deciding what kind of support will be provided. The IPP should also include a date by which the support will be reviewed to check how well the support is working and whether the outcomes have been, or are being, achieved.
- Do: The school or PUF provider will put the planned support in place. Your child's teacher or educational assistant would be responsible for working with them on a daily basis. The educational team should track your child's progress and check that the support is effective.
- Review: The support your child receives should be reviewed at the time agreed in the plan. This meeting will determine if the support is having a positive impact, whether the outcomes have been, or are being, achieved and if - or how - any changes should be made.
You should be kept directly involved and updated during this process, with your views, and those of your child, sought throughout.
Ready for School
Every child - including those with autism - has the right to mainstream education. Some children with more complex needs and disabilities attend specialized programs designed specifically to meet their needs. In the next section we will go through the different options and strategies on choosing a school.
Step One
In the Edmonton area, usually children must attend their designated or neighbourhood school and the school will put appropriate support plans in place for the child. If you are moving to Edmonton, it is advisable that you so some research to figure out which program or school is the best fit for your child. Some schools in the Edmonton Public School system have an autism specific program called Interactions. You can find out more about this program by visiting their website: https://www.epsb.ca/programs/specializedprogramming/interactions/
They also have other specialized programs that may be of interest to you and you can find out more by visiting here: https://www.epsb.ca/programs/specializedprogramming/
If you are choosing Interactions or another specialized program, please know that these programs fill up quickly and you will need to contact the school in January or February to look at a spot for the upcoming school year.
Step Two
Visit. Most schools have an open house, usually in early spring. Check the schools' web pages for open house information or contact the schools directly to ask. Draw up a list of schools to visit and go to as many as you can (you may need to book, so check first). This is your chance to get a feel for the school, speak to students and staff, and see the classrooms, playground, and facilities. If you have missed the open house opportunity, call the school to book an appointment for a tour to get a feel for the environment and the staff and ask questions about how the school will be able to support your child.
Step Three
Once you have decided on a school, see if you and your child can meet the teacher before school starts so that your child can get to know them and become familiar with the classroom before all the other students will be there. If there are accommodations that you think could help your child in the classroom environment, be sure to suggest them to the teacher so they can be implemented before the first day of school.
Step Four
Complete and submit your School Admissions Application form. Make sure that the school has copies of your child's diagnosis and relevant reports so that the school has as much information as possible in regard to your child's needs so that they can implement the best support.

101, 11720 Kingsway Avenue
Edmonton, AB, T5G 0X5
Treaty 6 Territory
Phone: 780-453-3971
Charitable Registration #
107282055RR0001
Autism Edmonton is a safe space that welcomes and supports all members of the LGBTQ2S+ community.